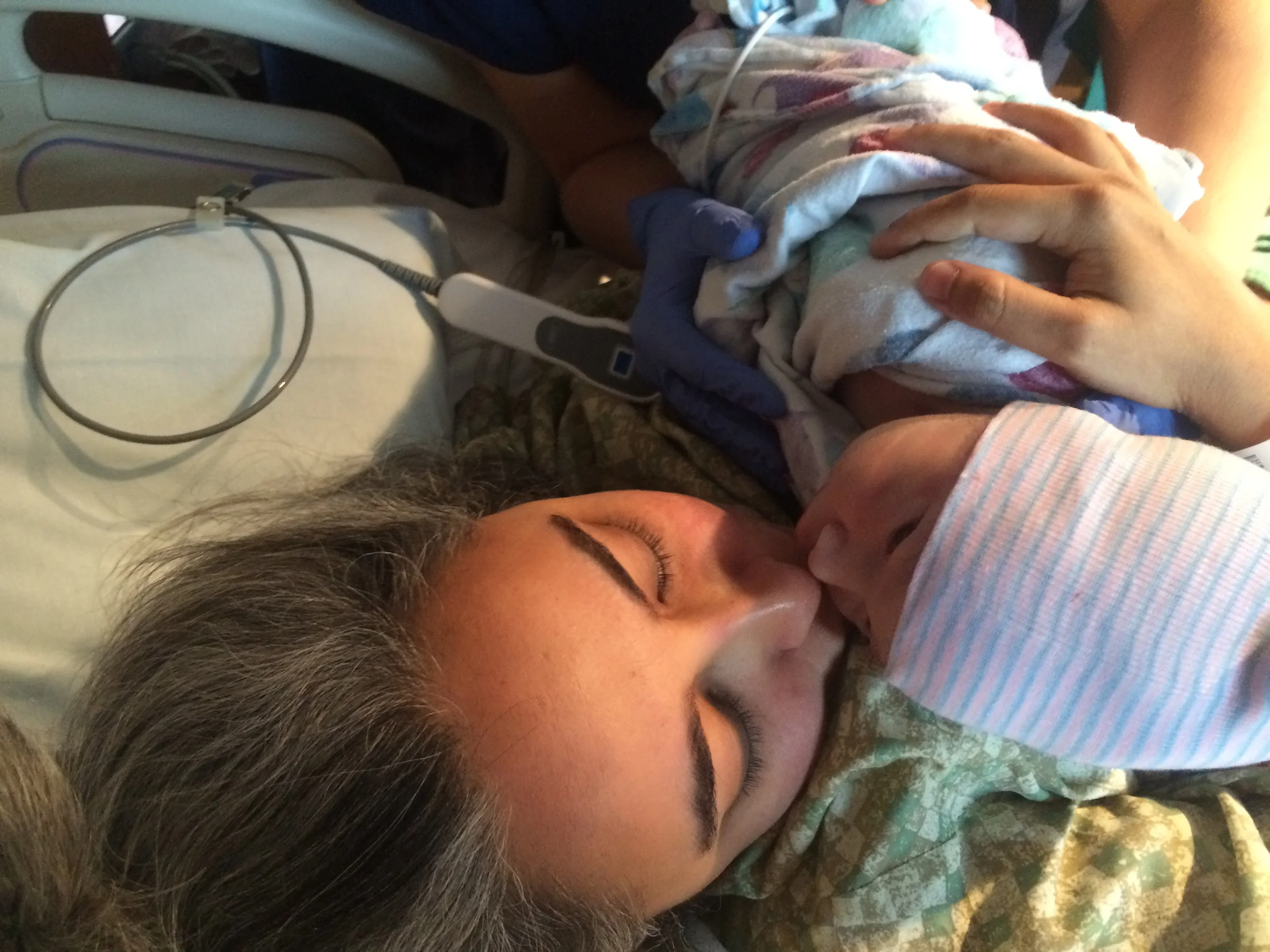
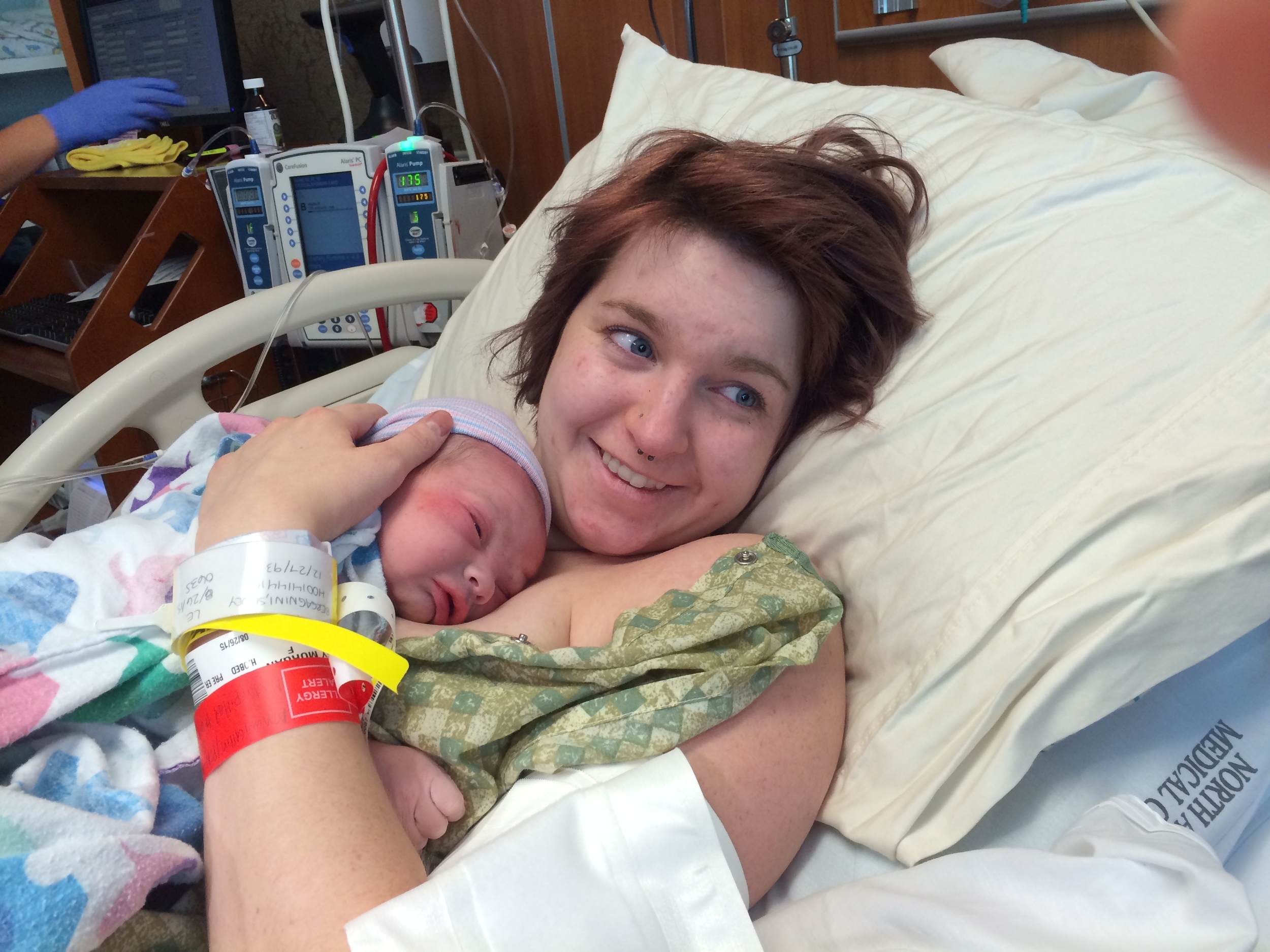
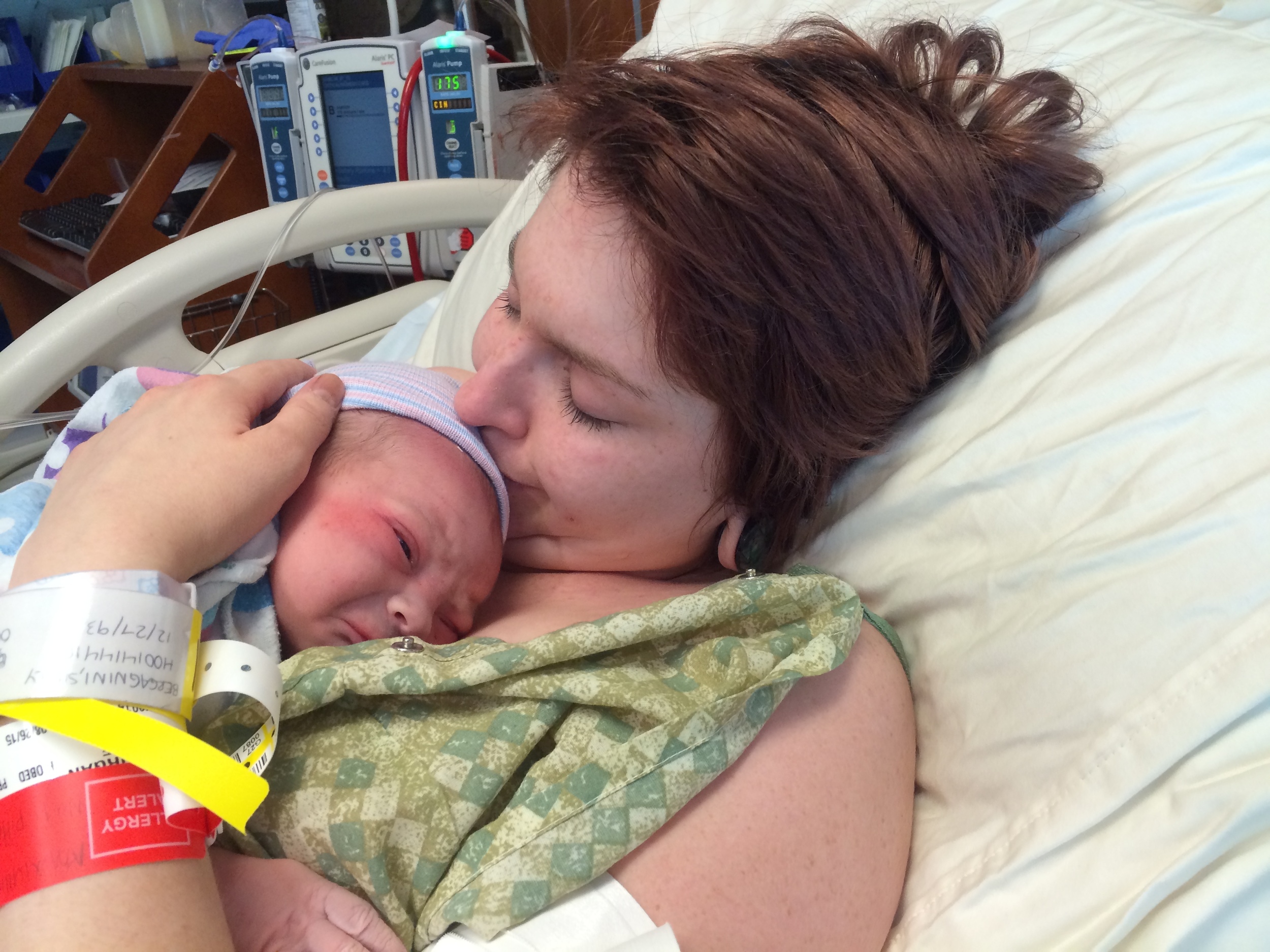
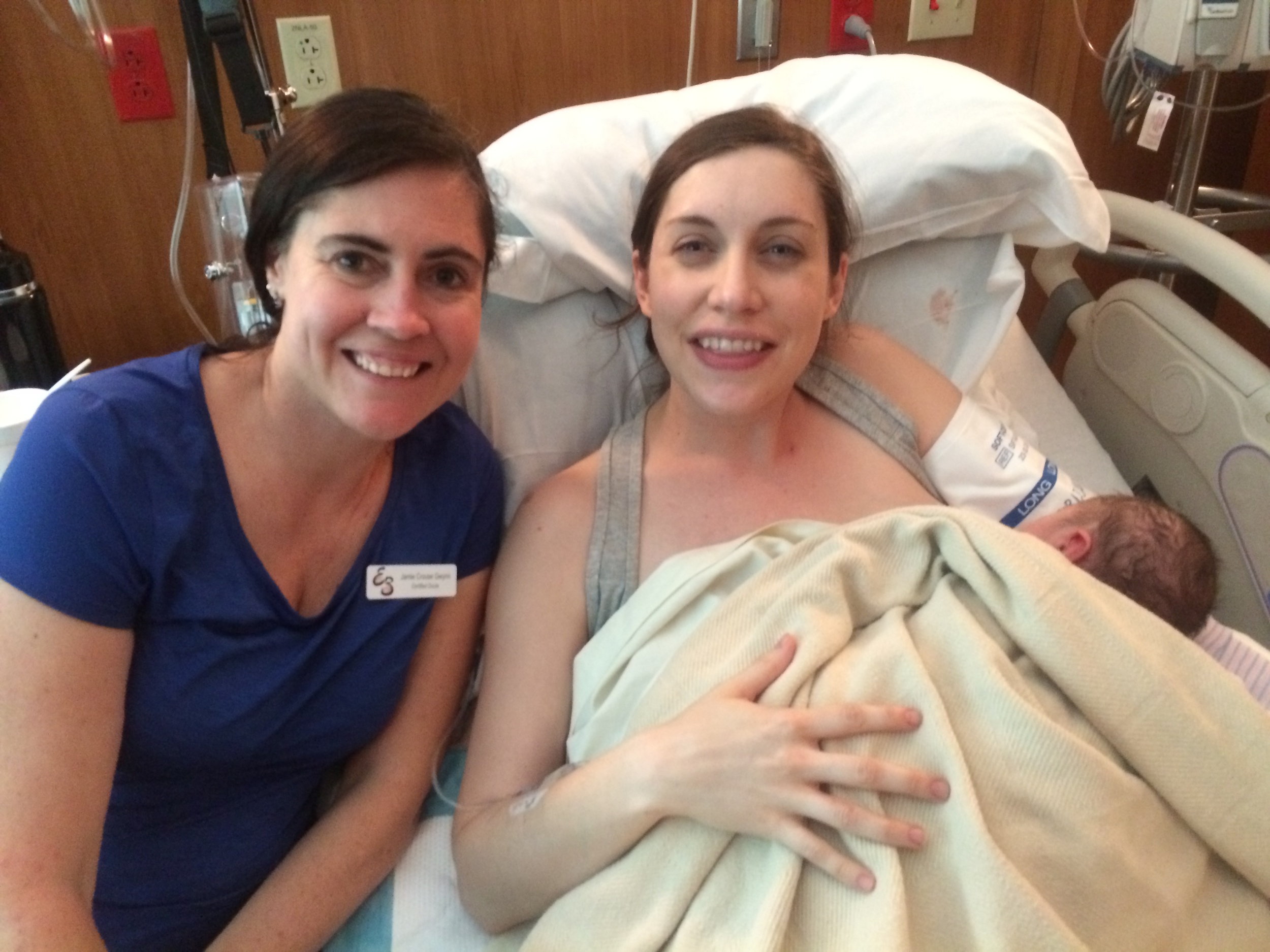
These beaming new parents, Sarah and Nick, welcomed their son, Eli Thomas into their arms on July 16 at 10:15pm at Natural Beginning Birth Center. Sarah did such a wonderful job through her long labor, with the loving support of her husband and patient midwife, and eventually all her hard work paid off and she achieved the gentle, natural birth she was hoping for. And she got this beautiful boy!
What the CDC Can Learn from Doulas
If there is one issue that stirs the hearts of doulas, birth workers, and birth activists of all stripes, it is informed consent. That presumes the existence of both information that is available and understood, and autonomy. That is, we believe women (and all birthing people) are capable and entitled to make their own decisions about their bodies and the baby they are carrying. But autonomy has a really troubling history in our culture. As far as the feminist movement has come in bringing women autonomy in their careers, in their sexuality, we still as a culture have a great distrust that women can make the “right” decisions regarding their unborn babies. Of course, this plays out in the in abortion debates: whose decision is it whether a woman maintains or terminates her pregnancy? We see it in extreme cases of court-ordered cesareans and women charged as criminals for suffering a miscarriage or stillbirth (yes, these are real). On the everyday level, birth activists get incensed around the language of permission that is so often used in birth and maternity care: “The hospital doesn’t allow you to eat in labor”; “my doctor won’t let me have a VBAC”; “If your baby hasn’t been born by 41 weeks, we will induce,” etc. ad nauseum. (See Birth Monopoly, "You're Not Allowed to Not Allow Me" ) All of this displays a deep distrust in women to make their own decisions. It is paternalismat its core: “don’t worry your pretty little head about this; the doctors, the scientists, the politicians (all historically male professions, even if they now admit women into their ranks) will tell you what to do.
Now enter the CDC’s recent recommendation that all sexually active women not on birth control from their first period until menopause refrain from all alcohol intake ever. The first I heard of this, it seemed laughable, like it must have come from an Onion article. But when I understood its reality, the anger set in. How dare they try to control the daily choices of women like this? How condescending! How paternalistic! And I am hardly alone in this feeling (See Birth Anarchy, The Atlantic, Salon, Forbes). I would like to give them the benefit of the doubt; they are actually concerned about preventing cases of fetal alcohol spectrum disorder in unplanned pregnancies, and they just didn’t realize how tone deaf their message was. But this only represents the prevalence of the paternalism surrounding women’s reproductive choices. Women are reduced to potential baby-makers, 33 million potential baby-makers, that is, 33 million potential babies are at risk of FASD.
So what’s wrong with this sweeping recommendation? Let’s break it down. First is that such a generalization leaves an awful lot of people and scenarios out. What about women who choose to be abstinent and are therefore not on birth control: they could get raped right? Maybe they shouldn’t ever drink either. What about those who have same sex partners? Do they need birth control too? Apparently, they forgot about them, but I guess a lesbian might be raped as well. What about women who rely on their partners to use a condom? Are the men responsible? (Probably not) What about the times when birth control fails? What about women who would terminate if they had an unplanned pregnancy? Maybe all women should just not drink ever, right? Maybe they shouldn’t drive cars either; they might crash and endanger the baby after all. At some point, it just gets ridiculous.
And what about all the women who for medical, religious, or personal reasons choose not to use birth control. What about women for whom birth control is inaccessible? Every form of birth control has its own risks, not only of failure, but of more serious side effects, such as blood clots (ie. the pill) or ectopic pregnancy (ie. an IUD). Whether to use birth control requires an assessment of risk. The CDC’s recommendation fails to take this into account. The risk of fetal alcohol syndrome is real, but the research isn’t as cut and dry as the CDC’s recommendation suggests. The language is actually that there is "no known safe amount of alcohol use during pregnancy" (my emphasis). This doesn’t mean even a single drop will cause harm, it does mean that we don’t know whether one drink is safe but five is not, and therefore it’s better to be safe than sorry. Some research has suggested low levels of alcohol is safe (see here) and other research points out the potential damage that even a little alcohol has on the developing fetus (see here). And this potential risk has to balanced against the risk of birth control itself, or we’re back to saying all women should never drink, ever. Risk is inherent. We will never get a state where there is no risk. So who gets to choose what risk an individual woman is comfortable taking with her body and her pregnancy?
This is where we come back to informed consent, especially the informed part. The CDC has an important role in educating the public and creating awareness around the issue of alcohol and pregnancy. So far, they’re doing a pretty good job. Almost all pregnant women or those trying to become pregnant know to avoid alcohol. We see the signs in the restrooms at every restaurant that serves alcohol. And with the exception of those dealing with addiction, compliance is pretty good. The CDC sees the need to further educate people who are not actively trying to become pregnant but might have unplanned pregnancies and who are still consuming alcohol. Then by all means, please continue to educate the public about the risks of alcohol use and pregnancy. And we certainly need work to make contraceptives safer, more affordable, and more available. But, most of all, let’s trust women to evaluate the risks and make an informed decision for themselves. This is where the CDC could learn from doulas. As non-medical professionals, we do not offer medical advice or recommendations, but we are experts at presenting evidence-based information in a non-biased way. We trust women and their partners to be able to evaluate that information and make the decisions that are right for them. If, as we believe, a woman is capable of weighing the risks of a VBAC and a repeat cesarean and making the decision that is best for herself and her actual baby, then she can also decide whether or not to have a glass of wine with dinner.
Valentine's Newsletter
Do you believe in love at first sight? I do. I witness it every time a new family lays eyes on their baby for the first time. I love what I do. I love being part of this miracle, of being invited to participate in the first moments that you have together. I love seeing your love, your joy, your strength, your determination.
It has been another wonderful year of serving families through Empowered Birthing. It has been my privilege to serve eleven families through their birthing journey in 2015, and another three families this year. I have witnessed a great variety of births: VBACs, twins, hospital births and out-of-hospital births, cesarean births, natural births, marathon births, and fast intense births. But in each one, I have seen mothers calling on their deepest strength to bring their babies into the world.
Through each birth, I learn more about the wonderful process of birth. I have also had the opportunity to expand my learning in more formal ways in order to expand the services I provide. In the summer, I completed my training as a Go Diaper Free Certified Coach. Through this program, I solidified my interest and learning about Elimination Communication (aka infant potty training). I have started a monthly support group for families practicing EC, and I am available for private consults as well. If you are interested in knowing more about this, I would love to share more. One of the most valuable workshops I have been able to attend was with Spinning Babies, which teaches us how to support optimal fetal position for easier and faster births. It really has revolutionized my doula practice. I was also able to attend a training with Susan Steffes, a specialist in women’s pelvic physical therapy, where we learned many ways to support women’s pelvic health through pregnancy, birth, and postpartum. I was also able to learn more about Postpartum Mood Disorders through a workshop with Postpartum Health Alliance of Central Texas. And just last month, I embarked on my recertification process with DTI (Doula Training International) as a birth and postpartum doula. I am very excited about my new connection with DTI, which more closely aligns with my philosophy. They are strong advocates for improving the maternity care system and for women’s (and doulas) autonomy, and committed to fostering a strong sense of community. I am happy to be affiliated with this organization, and I look forward to growing with them. I am also excited to begin expanding my postpartum services.
I love the work that I do, and it has been an honor to support each and every family that I serve. I really pour my heart into helping you achieve the best birth possible. I hope that you will share the love and consider writing a testimonial about your experience with me and by sharing with your friends about my services. Please keep in touch. It is always a pleasure to hear from you, see pictures of your babies, and help you with any parenting questions you may have. You are welcome to follow me on Facebook, both personally and my business page at https://www.facebook.com/Empoweredbirthingaustin/.
Happy Valentines Day! May you and your family be blessed with an abundance of love!
This is what love at first sight looks like!
My new DTI tribe!
Welcome Baby Isabel!
Congratulations to Lisa and Steve on the birth of their daughter, Isabel! Isabel was in such a hurry to meet her lovely parents, and after only a couple of hours of labor, Lisa arrived at the birth center fully dilated. Dad said that her middle name would be "Freight Train." But Lisa coped with the intensity of a fast labor beautifully, and had such a beautiful, gentle birth. It was an honor to be part of their birth!
What a beautiful new family!
Spotlight on Austin Area Birthing Center
Austin Area Birthing Center is the oldest and largest birth center in the Austin area. It was founded in 1987 with its first location on Duval Rd, now the North location. They expanded to include a South location in 2011, and just this month have opened a third location in Cedar Park. Each is designed with bed-and-breakfast style, themed birthing rooms, equipped with a large birthing tub, showers, and bed as well as a clinic, family waiting room and classroom space. They have really gone above and beyond to create a space that is comfortable, peaceful, and luxurious but also combines all of the necessary tools for giving birth.
Barcelona Room at North Location
Where AABC really shines though is in the care of its midwives. AABC employs both CNMs(Certified Nurse Midwives) and CPMs (Certified Professional Midwives) and they all work well together as a team without any apparent in-fighting (which is unfortunately not always the case in the birth world). Although each midwife brings a different personality and style, there is consistency in care across the board. Since I birthed both of my two sons there, I can testify to the high level of care that I always received. Midwives spend plenty of time at each appointment listening, answering questions, and providing personalized care. Even in such a large practice, I was surprised that I was always recognized and remembered, even though there were some midwives I did not see as frequently. There is a consistent effort to make sure each client receives is treated warmly, professionally, and individually. I found care there that I had never experienced from any other medical professional. Also for a large staff, I rarely ever had to wait more than a few minutes for appointments, and office staff responded to questions promptly. In the birth, some midwives have a more hands-on approach than others, and some give more direction that others, but birthing mothers are always encouraged to lead the way in how they want to labor. When all goes well, birth is calm and peaceful, and mom is never separated from her baby. In emergencies, (and as a doula I have witnessed this) the midwives are expertly trained and handled the situation with poise and quick skill. And for anyone who is concerned, each location is within a few minutes of a hospital, and all necessary equipment is on hand to handle an emergency (short of a cesarean).
One of the advantages of being with a large practice like AABC is all of the additional classes and community events that are provided for clients. Everything from birth classes, prenatal and postnatal yoga, infant massage, breastfeeding support, and postpartum support groups. There is also a lively on-line community of AABC families. Clients have the option of doing Centering Pregnancy group rather than individual appointments. This fosters a sense of community, and gives much more time for education about pregnancy, birth, and postpartum as well as providing individual time for monitoring mom and baby’s health and progress. On the other hand, a large practice does mean that you will not be able to form the same kind of relationship with a particular midwife as you might at a small birth center or with a home birth midwife. And because they share call, you cannot know in advance who will be at your birth. However, for a large practice, they do an excellent job of creating a sense of community and involvement.
AABC has also recently expanded to include planned hospital births as well as home births, making it the most comprehensive birth center in the area. They CNMs at the birth center have gained admitting privileges at Seton hospitals so that during a transfer, the midwife can still maintain care for the client in the hospital, unless an assisted delivery or cesarean is needed. Since only the CNMs have this privilege, it will only be possible if there is a CNM who is currently available, but this is a huge advantage when it is available. They have also gained a partnership with an OB group out of St. David’s which will allow them additional transfer options. Planned hospital births are also possible for women who want midwife care but prefer to deliver in a hospital. The CPMs have also opened up the option for a home birth as well so that you can access all of the great community assets of AABC but you can have the birth in the peace of your own home if desired. Unfortunately, home birth is not covered by most insurance, whereas AABC accepts most insurance for the birth center births.
All in all, you will find lots of options, a great sense of community, and personal, individualized care at AABC in a really comfortable and beautiful space.
Check them out at www.austinabc.com.
Welcome Baby Eliot
Join with me in welcoming baby Eliot! I am so proud of mom's strength and determination through a super long labor and dad's caring support through it all. Congratulations on a beautiful baby boy!
It was such a joy to serve this fabulous couple and be a part of welcoming this precious baby boy!
The Birth Story of Claire Rosalia
It is my two-year doula-versary! Just two years ago I got to attend my very first birth as a doula, and I got to share in the welcome of a special little girl. This is her story:
Claire’s due date had come and gone. Long ago it seemed. Every day after October 16th I would start each day and each night wondering, “could this be the one?” But they would continue to pass just as the one before. After just a couple turns of the clock like this, my hope became stained with anxiety. I knew that many first time moms went past their due dates, and I knew that those dates are educated guesses at best, but still I started to worry. I had stopped going into work that Friday before and felt that I needed the baby to justify to them why I was no longer sitting at my desk typing emails from nine to five. I started to think that how each day off work without that baby was a day that I wouldn’t have her all to myself at the end of my leave. I also worried about that fourteen day mark that was ever growing nearer. What if I had to give birth at a hospital? There were so many unknowns to that scenario that I wasn’t ready for, things I never wanted to have to prepare for or think about.
I had been having Braxton hicks contractions for a couple of weeks already, which feel like a simple tightening of the abdomen (as if it wasn’t tight enough already!), and these quick and rather sharp cervical pains that I learned were likely the start of effacement. As with so many other things during the course of pregnancy, these feelings became the new normal after the first week or so of experiencing them. It was wonderful and reassuring to know that my body was gearing up for the big day and I enjoyed feeling each practice uterine contraction, each cervical pang, and each leg stretch from the little baby inside me, despite the worries and anxieties that I just couldn’t seem to squash. One way or another, we were going to meet this little girl soon!
Monday October 21st was the best day since my due date had passed. I went to see my midwife for a checkup and she really set my mind straight again. She reminded me with perfect conviction that it was completely normal to be late and that there was nothing to worry about. She checked me inside and out and was impressed with my general health, the baby’s health, and my body’s progress thus far in getting ready for labor. She seemed sure that we would have this baby before the week’s end. I let her know my fears of having to go to the hospital and she reminded me that if we did make it to that point after trying all of their tricks to stimulate labor for all of those days, I would be ready for that option. A midwife would go with me to the hospital to navigate the protocols and be my liaison to help me get the best birth possible. She gave me some ideas for getting things going and sent me on my way. I felt a million times better after that. I went home relaxed, happy, and willing to wait it out until Claire was ready to greet the world. Trying every trick in the book that I learned from the midwife, the grapevine, and Google anyway, just in case. I had to feel like I was doing something to encourage this show to get on the road. If it was baking spicy gingerbread cookies and watching a weepy movie that just happened to be the ticket, then I would leave no stone unturned!
The contractions I was feeling were starting to get more noticeable and more frequent by midweek. Days passed like this, but still there was no rhythm to them and they weren’t strong enough to take much of my attention. I would announce them to my husband and mom (at their request), but even that got old after a while. ‘Yup, guess what? I am having another contraction. Big Whoop.’ Some of them came with a new dull ache that felt like period cramps, and a couple of them I felt in my back. Then, on the evening of Thursday October 24th while sitting on the couch with my mom, I felt like the contractions had started to take on a rhythm and got a little “spicier”. I downloaded an app (which was a great idea!) and started timing them. They would ramp up relatively slow, keep a little plateau of feeling at the top, and then so very slowly ramp down until all I could feel was the tightness in my uterus but no sensation other than that. For a few hours they were about 30 seconds long for anywhere between 8 and 15 minutes apart. Now THIS really could be the night!
I decided to go to bed since it was now about 11pm or so and I had been taught to get sleep if I could just in case it was the last chance I had. A couple of contractions woke me up while I was sleeping, but it wasn’t until 3am that I realized I had been having contractions for the last hour that I could no longer sleep through. The sensation of them was getting stronger now! Excited, I hopped out of bed and told my mom that I was having regular contractions that seemed to be about 6 minutes apart. She hadn’t slept a wink yet, probably as excited as I was trying not to be about all of this activity. I timed a few more contractions while sitting on a birthing ball in the living room, my excitement growing as they came almost on cue and showed no signs of relenting. They were now only a few minutes apart, but became irregular between 2 and 5 minutes apart. I counted them as lasting between 30 seconds and a minute. There was no doubt about it now, this was definitely going to happen today. I decided to take a shower and gather some last minute things for the birthing center.
At 4:30am I called the midwife and our Doula, Jamie, to let them know what was happening. The midwife that called us back let me know that I was in the earliest stages of labor still and that if I could make calls and answer questions, then it was still too early to go anywhere. She must have been right, because I found myself talking to her through a contraction or two while I had her on the phone. The sensation was bordering on pain now, but it was still very manageable. She let me know that I was looking for the contraction to take all of my attention for a full minute, and be 4 minutes apart for an hour. I hung up the phone and woke my husband. It may not have been time to go anywhere just yet, but it would surely be soon and it was time for all hands on deck.
Jamie showed up about an hour later, at 5:30am. We weren’t sure until the week of my due date if we wanted a doula for our birth. When she came in the door, I was immediately happy that we had decided to get one in the end. I filled her in on the progress of the morning and she got to work; never leaving my side. Already, the contractions were getting stronger. We sat on the couch together, me switching between sitting up and laying down, and rode those waves that were coming now every 3-6 minutes and lasting 30 seconds to a minute. She helped me visualize the sensation as riding up a steep hill on a bicycle. Seeing the top coming closer and pushing through the discomfort of the effort, and then finally making it to the top and coasting down the other side, relieved and accomplished. This worked well at this stage, and I crested hill after hill knowing that the release was always soon to follow. At some point during this time, I started to vocalize each contraction. I had learned from birthing classes, prenatal yoga, and reading Ina May books that this can be a very useful tool. Using an “O” sound with your mouth can literally help to open you up down below. Using a deep voice rather than a high pitched one is said to help too, as well as keeping your face relaxed. I also concentrated on keeping my breath slow and deep, which the vocalizing helped with a great deal. I started using these tools almost automatically once the contractions became intense enough to need something additional to focus on. It was as if my voice was matching the power of the sensation in my back and lower uterus. Like an answer to a challenge; my power to its power. This method worked really well for me and I stuck to it for the remainder of the labor.
Most of the pain was in my lower back and hips, so I tried to do a lot of rocking on my knees or on all fours when I could manage it in case it was because Claire was faced the wrong way in my pelvis. But my body was tired already, so it was difficult to prop myself up on my arms for too long. I had taken to closing my eyes, going inside myself and taking each contraction at a time, resting as much as possible in between. Jamie was behind me for every one, pressing in on my back and hips – this was also something that I needed for each and every contraction until the end. It became necessary to have that counter pressure on my pelvis to get through them.
At 9am we called the birthing center again. The midwife had been right; at this point there was no way I was going to talk on the phone and I hoped no one expected me to be able to answer any questions. I needed to not be distracted by the outside world any longer. The contractions were now lasting a full minute and were coming every 4 minutes or less and had been doing that for right around an hour. I could feel the sensation of each contraction radiate through every part of my body now, though they were certainly concentrated around the middle of me. I think we were all anxious to move into the room where we would have this baby. They cleared us to come in and Paul and my mom went into a flurry of activity gathering food and drinks, the overnight bags, and stuffing everything in the car. We took two cars there, Paul took ours with the car seat in the back and my mom took her little rental with barely enough room for me to lay in Jamie’s lap in the back. By now I was in it! My eyes remained closed as I breathed through each contraction and in anticipation of the next. It was too hot, too bright, and I could not get into a good position. Even though I wasn’t looking, I knew the route so well that I could tell exactly where we were at each moment, each turn of the journey to South Austin. It felt like an eternity and I wanted so badly to get out of the car.
Once at the birthing center (about 9:30am), my family quickly unpacked and Paul’s parents showed up. The midwife checked my cervix and announced that I was only 1 ½ cm dilated. No it couldn’t be!!!! I was heartbroken at this news and wondered just how long this day was going to last. The midwife could also tell that I was exhausted from only sleeping a couple of hours the night before. It was tough decision time. She let me know that in order to avoid me wearing out before enough progress was made and us having to transport to the hospital, she could give me a mild pain med that would hopefully relax me enough to take a nap. And either way, we were going to have to return home to labor until I was 4-5 centimeters dilated. The last thing I wanted to do was leave there! Returning home felt like backwards progress and I didn’t know if I wanted to try and handle TWO more car rides. One was hard enough to take. The fact that I even was expected to make such an important decision in my state was surreal in itself. Maybe if I just laid there with my eyes closed and retreated back inside myself, she would go away and we could continue with the rhythm of the contractions. But I knew she was right, even though I asked her two or three times just to let us please stay. It was true that I was exhausted from laboring thus far, and I could hardly keep my eyes open to listen to her options for us. That, and since we had landed at the birthing center, the contractions had faded a bit (though I was only told this, I didn’t notice a change myself). I decided to take the mild pain med to see if I could sleep. I wasn’t happy about having to make that decision, but it was what would save us from having to go to the hospital, and somehow that was my greatest fear of the day.
Paul’s mom, Janie, had the marvelously amazing idea of us going back to their house to labor, since it was on the same side of town and so much closer. Somehow I was stood up, put my shoes back on, and tried to hide as much of myself in my hoodie as I could as we ambled back out into the bright, hot world and into the cramped little car for another impossible car ride. At their apartment, it was now about 11am. I laid down on the guest bed and tried to feel sleep coming on or those pain meds that I had just been shot with. The problem was that though I did feel drowsy for a short time and I did get a few longer breaks between contractions which probably only amounted to a few extra seconds each, I never got this “nap” everyone was hoping for. Not even close. In fact, we only stayed at the house for a couple of hours. I would lay on my side and relax as much as possible, breathing deeply, until a contraction would send me shooting up on all fours to rock it out (still thinking maybe Claire was turned the wrong way and I wasn’t taking any chances either way.) Things really picked up at about 12:30pm and I no longer felt much of a break between contractions. My voice became louder and louder in response to the ever increasing waves of sensation that shook my body. It was apparent that this labor was moving ahead whether we were ready or not, especially when a few of the last contractions gave me the urge to push! Jamie and my mom could hear it in my voice. I didn’t even have the luxury of being tired any more, and it soon became clear that we needed to call the birthing center and get the ok to make our way back.
We arrived back in the room at 1:30pm. Upon being checked, the midwife announced that I was 7-8 cm dilated now. Oh my GOD that was good news to hear. We had made so much progress! Granted, I had absolutely no concept of time throughout the whole day and I did not know how long we labored at Paul’s parents or what time it was at that point. Godzilla could have trampled all of downtown Austin that morning and I wouldn’t have known nor cared, as long as it didn’t get in the way of my immediate world of careful laboring. All I knew was that somehow I had opened up and we were getting so very close to meeting this baby of ours. It didn’t really occur to me at the time that the centimeter reading meant that I was in the middle of transition and had been for the car ride over. All I knew was that I could handle this. I was handling this. I was so close. What was 2 more centimeters? The bath was run and I quickly stripped the rest of my clothes off and gingerly got in to kneel down on a towel. The water felt warm but didn’t provide the relief I always hoped it would. At this point, there was only a few breaths between each long contraction, which I met with a now furious roar that came out with each long exhale and had me almost gasping for breath in between. I couldn’t believe the strength of the noises coming from my mouth. It made me feel powerful. It gave me a sense of awe for the power of my body; a respect for what it could do all on its own. I knew with each contraction that it would rise but then it would fall. I would get a few precious seconds of relief to recover and ready myself for the next one. It was the most intense physical pain I had ever sustained willingly and consciously, but I was never fearful of it. Especially since I knew we were so close. Jamie was in the tub with me, standing and pressing on my back. I would direct her hands to the right spot if she was off a little. Paul got in front of me on the counter and I found both his hands and clutched them desperately through the contractions. I wanted him to feel the intensity of what I was going through. My eyes remained shut and it was harder to keep my face relaxed, though the open mouth roaring really helped me relax as much as I could manage. Some of the contractions made my head rise up and my back arch in response. I felt the strength of my arms and my legs holding on for dear life. The last ones gave me that urge to push again and I could hear waves of agreement around the room when they heard it in my still rising voice. They told me to try and shorten my breaths, which I tried but had no idea if I was doing what they meant and if it was making a difference.
In 20 minutes I was checked again. I was fully dilated with just a little lip left to go! I was almost there! The midwife announced that I would have to move to the bed to push since I had progressed so quickly. They needed to be able to get a better view of what was happening and to make sure that I wouldn’t tear. I wasn’t happy about this; I think I had imagined having this baby in the tub, with my husband in it with me. But they knew best. I did the next couple of contractions with the midwife’s hand inside me to lift the last lip around the baby’s head. Then, it was time!! Moving out of the tub proved difficult, and I had to stop twice to let a contraction pass - once with one leg in the tub and one leg out, and once standing in front of the bed before I was able to get on. I felt like any major movement at this point brought on another contraction. It made me hesitate to move much unless I had to. I could also feel the baby low in my pelvis, and the widening pressure of her head bones squashed between my hip bones also made it difficult to move too much. The last thing I wanted to do with my legs was close them to perform actions such as walking or crawling on the bed. It wasn’t a painful feeling, just awkward and I didn’t want to run the risk of squeezing her little head any more than I was already or pushing her back up into the uterus.
I was back on the bed and ready to push at 2pm. I tried hands and knees, on my knees with Paul in front of me so I could hang on his neck (and scream in his ears which were surely ringing by now), and on my back but cocked to one side with one leg up. On my knees with my arms wrapped around my husband was the best feeling in the world at that moment. Knowing that he was right there, taking my weight and my screams and experiencing everything through me was an amazing bonding experience for both of us. Feeling the strength of his body gave me strength. I could actually hear people around us agree that it was a beautiful sight to see, as I buried my head in his neck during my recoveries. For over an hour I pushed; only getting 3-4 exhales of pushing before needing to recover for what seemed like 10 breaths. It was such exhausting work! Much tougher than any of the contractions before. Each time my long recovery started, I breathed deep and slow, knowing that I would have to give it even more the next time…and I was so tired. During this time more people came into the room. A new midwife instructed me to stop letting out so much of my energy through my mouth now. I would have to bear down instead, and send all of the energy to the bottom. I tried this and it worked beautifully. I gritted my teeth and grunted, visualizing my energy moving downward rather than upward, which is where it had been going for the last however many hours it had been.
The extra people in the room were there for a reason. I knew that something was up and that the midwives and assistants were not alarmed, but they were on high alert. They didn’t let me know what it was, and I started having inklings of worry toward having to go to the hospital again. I felt like I had been pushing for so long – hours – what if I didn’t have the energy to get her out? An oxygen mask was put on over my face and I heard something about the baby’s heart rate. Turns out it had dropped a few times and they were just monitoring it extra carefully in case it turned into a situation worth acting on. Still I pushed. I pushed and I pushed, recovering deep and long and slow in between. I could feel the stretch and tightness of her moving down inside me, and I was hoping for someone to call out, “the head!” but I heard no such thing yet. Push Push Push! Loooong Recovery. Push Push Push! Loooong Recovery. I had been moved from my back to my knees and again to my back. Paul was behind me and I was gripping his hands; Jamie had my left leg in her arms to hold it up. I was instructed to curl my body inward rather than arch my back while pushing. I dutifully did so. I had a room full of cheerleaders all around me encouraging me on. “That was a great push, let’s give it one more!” “Yes, like that, keep on pushing!”.
Finally, someone saw the head. It was full of dark hair! I could see it in my mind. I gave it a couple more rounds of pushing and felt the stretching sting of her head make it through. So many hands were on me, protecting me and the baby. She had come down in the right position. I paused to let them check things and then pushed on command. For the last time I pushed. Immediately out gushed the rest of her body, so fast that it surprised everyone. It felt so small and slippery compared to that head. They lifted her up and set her on my chest, all warm and slippery and bloodied. I could feel the warm tug of the cord that still connected us between my legs. She cried and I was in complete shock, my eyes now wide open. A million emotions flitted through me as I held onto my daughter for the very first time. I looked up at Paul, who was crying and looking on at her. The midwives covered us with a blanket, put a little hat on her, and got busy cleaning me up (there was a lot of blood, but I had been prepared for that so I didn’t mind.) The energy in the room was so incredible. Cameras came out, and everyone was buzzing with wonder, relief, and happiness. I kept looking from her to Paul and back to her. Our new family.
All in all it seems that I was in labor a total of 13 hours, (starting from the contractions that kept me awake at 2am), with active labor only lasting a short 3 hours. I did tear a little bit when her body came out so fast, but it was an internal tear and it just took a few stiches. I didn’t even feel it when it happened, and they numbed me to stitch it up.
Claire Rosalia Garcia weighed in at 6 lbs and 10 ounces, was 19 inches long, and extremely healthy and happy. She didn’t cry much, and almost immediately took to the most important task of eating. She took to my breast right away (with some help from the experienced ladies in the room) and fed for over an hour, which is always a good sign. I couldn’t have been happier with how everything went. Already I started to recount the events of the day, in awe of my very own birth experience. It was an incredible, intense, epic journey that I couldn’t believe I had just accomplished. All of those hours of reading, yoga’ing, studying, and prepping really paid off and helped to empower and comfort me. Knowing that each contraction, each sensation, and each hour every step of the way was all part of the process. All natural, normal, necessary, and most importantly, perfectly surmountable pieces to getting my beautiful baby girl out and into the world.
Welcome Link Anthony!
Join me in welcoming Link Anthony into his parents' arms. Sidney made labor look like a walk in the park, and when it was time to push this petite young woman was a powerhouse and roared her baby out. Congratulations Sidney and Seth! It was a pleasure to work with you.
Rorie's Birth Story
This little guy just had his first birthday, so I thought it would be a good time to share the amazing story of his birth.
Amber was expecting her third child. With her previous births, she had elected to use pain medication but had had bad reactions, so this time she was determined to have a natural childbirth and let her body do what it was capable of doing without interventions.
Her husband was in the military and was stationed out of state, but Amber hoped and prayed that he would be granted a leave to come home for the birth. And as we were quickly approaching her due date, his leave was granted for ten days. So we prayed that her labor would hold off until he made it home, and it did! But then the days of his leave were passing by, and we still didn’t have a baby yet, so we prayed for labor to start, and we began trying a few natural methods to get labor going, but nothing was working. Amber reluctantly consented to an induction so that her husband could be present for the birth, but we were still hoping for labor to begin spontaneously. Her induction was scheduled for Sunday morning so she checked in the night before.
And from here on out, Amber tells the story in her own words:
“I went in to the hospital around 10 pm. I was scheduled to be induced the following morning. My OB wanted me to start the IV with Pitocin at 5am. I was a couple of days past my estimated due date. I had spent the last week trying natural induction methods and they didn’t seem to be working. I was only 1 cm dilated and maybe 20% effaced at that time. It didn’t seem as if I was close to natural labor at all.
When I was admitted to labor and delivery, I immediately asked the nurses if I could try induction with the foley bulb. My doula, Jamie, had me look into that as an alternative to Pitocin. After I read into it, I decided I wanted to try that first. Unfortunately, the doctor wanted to stick with the Pitocin in the morning so my request was denied. The nurses got my husband and I settled in a room and the nurse have me some melatonin to help me fall asleep. I fell asleep a little before midnight.
At 2am I woke up with some mild contractions. They were the first of any painful contractions I had felt throughout the pregnancy. I tried to fall back asleep but them at 2:30am I got out of bed to use the restroom. That was when I noticed I was losing my mucus plug. I started to get a little excited. I was hoping I would go into labor completely naturally. I called the nurse and told her that I was experiencing mild contractions and she came to monitor them.
At around 3am I noticed fluid leaking. My water was slowly breaking. The nurse had me on the monitor for about 30 min but I didn’t have any contractions at all during that time. I was a little discouraged but I asked for a birthing ball.
I bounced on the birthing ball for a while listening to praise music and praying. Soon I started experiencing more mild contractions. It was a little after 4 am. The nurse came and checked me around 4:30 because they wanted to start the Pitocin at 5am. I was dilated 2-3cm.
By 5am I was having painful contractions and they were getting regular about 5 minutes apart. I thought it might be a good idea to let Jamie know that I was going into labor. I told the nurses I did not want any Pitocin and I was sure my body was doing everything on its own. It was such a wonderful feeling to know that! My contractions became stronger and I became very nauseous. I began to throw up during and after every contraction. It made the contractions seem unbearable. I asked the nurse for something to help with the nausea. She gave me Zofran and it helped a bit. I tried laboring in different positions, including the birthing ball. I found that the only position I could tolerate my contraction in was standing, rocking side to side and leaning forward into my husband.
Jamie arrived to my room a little after 6am. I was still nauseous so she pinned a cotton swab with peppermint oil to my top, it helped and was refreshing. My contractions were very painful and Jamie helped my husband apply pressure to my lower back during them. It helped so much! Around that time the nurse checked me again and I was 4-5cm dilated. They put me back on the fetal monitor. My contractions became closer together. The baby’s heartbeat would drop with the contractions so the nurses had me try to labor in different positions. I tried lying on my side in the bed but it was too painful and felt very uncomfortable. I stood back up and next to me bed. The contractions were coming so quickly.
The doctor came in to check on me. I was in so much pain and I became very afraid. I didn’t think I could do it anymore. Jamie and my husband assured me I could. Jamie told me I was very close. Soon after that I felt an urge to push. The doctor began to put on her scrubs and gloves. I really had to push and I was still standing on the side of my bed. I was finally ready. It came so fast! The nurses raised my bed and the doctor sat on the floor. I felt so much pressure. The baby’s head was crowning. I continued squatting on the side of my bed andafter a couple of pushes he was out. He was born at 7:05 am. They had to cut his cord immediately because it was around his neck and then they gave him to me. I was still standing next to my bed. I held him to my chest, completely in shock. It was the best feeling. I smiled and laughed."
We were all so happy that her prayers had been answered. Her husband was able to be present, and Amber had the beautiful, natural birth that she was hoping for. She did an amazing job as she coped with a very fast and intense labor, and her body did it all on its own, in the most perfect timing.
Congratulations Amber and William, and happy birthday Rorie!
Welcome Liam Connor!
Congratulations to Michelle and Collin on the birth of Liam Connor! This cute 9.5 lb, red-headed little Irish baby made his mama work 40 hours for him. What a warrior mama! I am so proud of her determination through it all! Thanks for letting me walk this journey with you.
Welcome Elan Able!
Join with Shelby and Tyler in welcoming Elan Able. This precious little guy was in such a hurry to meet his mommy and daddy that he came a few weeks early and barely waited for them to make it to the birth center. Although it was a rush, mommy got to have the peaceful waterbirth that she wanted at Birthwise Birthing Center. He is happy now that he is in his mommy's arms. And now that he is here, I am excited to also help Tyler and Shelby begin their Elimination Communication practice with Elan. Congratulations Shelby and Tyler!
Welcome Luna Kinsley!
I'd like to join Sara and Andy and big brother Caeden in welcoming Luna Kinsley! Sara and Andy did a great job in preparing for this birth so that they could have a better birth experience this time. And sure enough, this labor was very different. Sara had a fast, intense labor and arrived at the hospital just in time to push this little girl out, who was so anxious to meet her family. Even though it was a little crazy there at the end, Sara got the natural VBAC that the wanted, and Luna was welcomed into a loving arms. And now they are on the crazy adventure of having two under two. Congratulations Sara and Andy! It was a pleasure to work with you!
Congratulations Stephanie and Mike!
Stephanie and Mike celebrated the birth of their second child. They decided to let the gender be a surprise, so there was much shouting and celebration when their little BOY, Alexander Gene was announced to all the family. Little Alex weighed in 7 lbs 12 oz. and 20 1/2 inches long. Stephanie had a long and difficult labor but she stayed focused on her prize, and she had a beautiful and healing VBAC. She could hardly believe she had really pushed that baby out all on her own!
Every once in a while I get a chance to snap a photo just as mom looks at her baby for the first time. This is the expression of pure joy!
It was a joy to work with this family and be part of this joyful, healing birth. Congratulations Stephanie, Mike and big sister, Kaitlyn!
Welcome Elijah Charles!
Rebekah and Ryan welcomed their first child into the world, a boy, Elijah Charles at Austin Area Birthing Center South. This healthy boy weighed in at 8 lbs 4.5 oz and 21 inches long. His parents are overjoyed at his arrival. Rebekah's labor began with her water breaking 38 hours before the birth, so it was long and tiring but Rebekah did an amazing job coping. Fortunately she had a patient and wise midwife who helped Rebekah to follow her body's lead. Rebekah had been interested in birth, especially natural birth, since she was a little girl, and she got to have the beautiful and empowering natural birth that she had dreamed about for so long. It was such a pleasure to work with this sweet couple and help them on their journey to parenthood. Congratulations Rebekah and Ryan!
Welcome Luke Edward!
Congratulations to Abby and Danny as they welcomed their second child into their family, Luke Edward! Luke weighed in at 8 lbs. 4 oz. 20 3/4 inches long. Abby pressed through a long labor, managing her contractions with confidence in her body and herself. Just as she had wanted, she gave birth completely naturally, with no pain medications, and welcomed her baby with joy and love. She was supported by her loving husband, who believed in her and encouraged her each step of the way. And older sister Zoe, was enamored with her new little brother.
Happy Birthday Camilla!
Ilyse and Brandon welcomed their beautiful daughter, Camilla June on May 5, 2015. This lucky baby was born on her due date, 5/02 at 5:02 pm. Granddad joked that he was going to go play the lottery and bet on 502. Mom did a beautiful job coping with the intensity of labor using her relaxation techniques. She was doing so well we weren't always sure when a contraction came. We are all proud of her for achieving the natural birth she wanted. She was supported by her loving partner and her mother throughout her labor, and she was rewarded with a healthy and beautiful baby girl.
Congratulations Ilyse and Brandon! It was a pleasure to work with you.
International Day of the Midwife
It is International Day of the Midwife so I would like to take a moment to send my appreciation to all the midwives out there who are working tirelessly to normalize birth. I love midwives. I loved giving birth with midwives and I love working with midwives as a doula. When I first chose to give birth at a freestanding birth center, I don't think I had a whole lot of expectations about what midwifery care would look like, I just knew I wanted a natural, non-hospital birth. But I soon realized the care I received there (and this was a big, busy birth center) was different than any doctor's office I had been at. My care was so personal and individualized. I was always given options and expected to take the lead in my decisions. There was never a sense of "well this is just the way we do things." I got to know each of the midwives and they got to know me, and after my last postpartum visit, I began to miss my time there (Who ever misses going to the doctor?) And at my births, I felt wonderfully supported, encouraged, and lovingly cared for. It is because of their care that I eventually chose to become a doula, and perhaps one day, I'll journey down the midwifery path myself.
I think this chart about the midwifery model of care sums it up well.
The Midwife Model of Care
Definition of Birth
- Birth is a social event, a normal part of a woman's life.
- Birth is the work of the woman and her family.
- The woman is a person experiencing a life-transforming event.
Birthing Environment
- Home or other familiar surroundings.
- Informal system of care.
Philosophy and Practice
- See birth as a holistic process.
- Shared decision-making between caregivers and birthing woman.
- No class distinction between birthing women and caregivers.
- Equal relationship.
- Information shared with an attitude of personal caring.
- Longer, more in-depth prenatal visits.
- Often strong emotional support.
- Familiar language and imagery used.
- Awareness of spiritual significance of birth.
- Believes in integrity of birth, uses technology if appropriate and proven.
If you have a low-risk pregnancy, consider choosing midwifery care for your pregnancy and birth, whether you choose a hospital or out-of-hospital birth.
Samantha, the midwife who caught my firstborn
The Medical Model of Care
Definition of Birth
- Childbirth is a potentially pathological process.
- Birth is the work of doctors, nurses, midwives and other experts.
- The woman is a patient.
Birthing Environment
- Hospital, unfamiliar territory to the woman.
- Bureaucratic, hierarchical system of care.
Philosophy and Practice
- Trained to focus on the medical aspects of birth.
- "Professional" care that is authoritarian.
- Often a class distinction between obstetrician and patients.
- Dominant-subordinate relationship.
- Information about health, disease and degree of risk not shared with the patient adequately.
- Brief, depersonalized care.
- Little emotional support.
- Use of medical language.
- Spiritual aspects of birth are ignored or treated as embarrassing.
- Values technology, often without proof that it improves birth outcome.
World Doula Week
There is no better way to celebrate World Doula Week than by booking your free consultation!
Doulas Lower Cesareans By 60-80%!
Exciting new research has come out about the amazing benefits of having a doula. We have long known that having a trained doula present at birth leads to many beneficial outcomes, such as less use of pain medication, less use of Pitocin to induce or augment labor, greater number of spontaneous vaginal deliveries and fewer assisted deliveries and cesareans, better success with breastfeeding, and higher satisfaction with the birth experience. Previously, results have shown about a 30% reduction in cesarean rates with a doula present, but the newest research more than doubles these findings. This research is presented in American Journal of Managed Care in August 2014. Their study surveyed over 2400 women who noted whether they had received doula care, wanted doula care but did not receive it, and those who did not have and did not want/didn't know about doulas. Only 6% used a doula but their outcomes in reducing number of cesareans were substantially higher; in the other groups the rates of cesarean deliveries were consistent with the national average around 30%. They found that women who utilized a trained doula showed a reduction in medically-necessary cesareans by 60% (which includes such things as breech presentation, placenta problems, fetal distress, and maternal health conditions) and as much as 80% in non-medically necessary cesareans (which includes such reasons as a prior cesarean, long labor, being past the due date, provider's fear of a big baby or narrow pelvis, or mother's fear of labor/birth)! In their words, "Doula support was associated with a nearly 60% reduction in odds of cesarean delivery and 80% lower odds of nonindicated cesarean delivery, compared with not having doula support." Based on these findings, the writers acknowledge the great benefit of having a doula present for continuous labor support. Not only does it lead to better outcomes and higher satisfaction, but it is a worthwhile financial benefit. Cesarean births cost on average $10,000 more than vaginal births, so the cost of hiring a doula is well worth the investment. They suggest that insurance companies should recognize the potential cost-savings that is rendered from using a doula and should start covering doula services. See the full article here.
How exactly does a doula help lower your risk of needing a cesarean delivery? Stay tuned for Part II.
If you are interested in lowering your risk of needing a cesarean, please invest in a qualified doula. Book your consultation with Empowered Birthing today.
Happy Valentine's Day!
If you have any surprises, I have openings in November!